RELATED Live.
- About us
- Find Hospitals
-
KIMA Doctors
- All
- Anesthesiology
- artificial joint center
- Breast and Endocrine Surgery
- Breast cancer and thyroid cancer center
- Breast Surgery
- Cardiology
- Cardiothoracic Surgery
- Cerebrovascular Center
- Colorectal Surgery
- dental and maxillofacial surgery
- Dermatology
- Endocrinology
- Gastroenterology
- General Surgery
- Genito-Urology
- Hematology
- Hemato-oncology
- Infection Center
- Internal Medicine
- International Healthcare Center
- Korean Medicine
- liver center/Pancreas and billiary tract center
- Liver Transplantation
- Neurology
- Neurosurgery
- Obstetrics & Gynecology
- Ophthalmology
- Orthopedic
- Otorhinolaryngology
- Pediatric & Juvenile
- Pediatric Allergy and Respiratory Diseases
- Pediatric Gastroenterology
- Pediatric Neurology
- Pediatrics
- Physical Medicine & Rehabilitation
- Plastic & Reconstructive Surgery
- plastic surgery
- Pulmonology
- Radiation oncology
- Rheumatology
- Thyroid & Endocrine Surgery
- Urology
- Vascular Surgery
- KIMA News
- KIMA Live
- Community
KIMA NEWS
- Effective strategy to completely block the spread of COVID-19 in Seoul St. Mary's Hospital -
- Regular treatments held good including chemotherapy for blood cancer like leukemia, immunosuppression therapy, and hematopoietic stem cell transplantation -
- The online edition of ‘British Journal of Hematology’ published on the 18th, a prestigious European journal in the field of blood -
- A modeling hospital of 'K quarantine' with the global attention during the pandemic -
There was news about the story of A (5), who was diagnosed with acute leukemia in New Delhi, India, and flew about 7,000 km to Korea on the Children's Day. As soon as she arrived in Korea, she was immediately transferred to Seoul St. Mary's Hospital of the Catholic University. After tested negative for COVID-19, she took chemotherapy in the sterile ward. This story verifies the excellent infection control system of Seoul St. Mary's Hospital, in which any infection in the hospital is perfectly prevented even in the middle of the pandemic.
While the world is all-out focusing on treatment and prevention against the spread of COVID-19, Seoul St. Mary's Hospital has been more committed to protecting blood disease patients whose immunity is deteriorated and vulnerable to COVID-19. At the same time, regular treatments including anti-cancer therapy, immunosuppressant therapy, and stem cell transplantation have been provided. Based on those efforts, the research result on the COVID-19 response strategy of Seoul St. Mary's Hospital (President Yongsik Kim) of the Catholic University, was published in a world-renowned international academic journal in the field of blood and got attention as it was the first time in Korea.
Since the first case of COVID-19 in Korea on January 20 this year, hospitals and clinics in Korea have taken various preemptive measures to prevent the occurrence and spread of COVID-19 in hospitals. As the number of domestic patients surged from March with the sense of crisis intensified about the spread within hospitals, major university hospitals in Korea and abroad started to implement strict policies against the spread of COVID-19 to minimize unnecessary treatments: limiting the number of new patients and surgeries, and performing virtual consultation and treatments for the patients who are from the areas exposed to the virus.
In March and April, when the pandemic crisis of COVID-19 reached its peak, the European Society for Stem Cell Transplantation released guidelines recommending that chemotherapy for blood cancer or stem cell transplantation be postponed unless urgently needed. Many hospitals in the United States also began to implement the policies to minimize chemotherapy and stem cell transplantation.
However, for the patients with severe blood disease, if the treatment is stopped or postponed immediately, the disease can be irreversibly worsened and lead to fatal outcomes. When the world's largest blood hospital restricts regular treatments, the impact can be enormous to about 15,000 patients with various blood diseases in the hospital and 9,000 outpatients while more than 50 stem cell transplant procedures are performed every month. So, Seoul St. Mary's Hospital established a preemptive COVID-19 preventative measures instead of reducing the treatment of patients with blood diseases. As a result, it was possible to completely prevent the spread of COVID-19 in the hospital and maintain all regular treatments for the patients with severe blood diseases.
The COVID-19 response strategy of Seoul St. Mary’s Hospital is ▶ Classifying patients with triage questionnaires ▶ Separating patients’ traveling line based on the triage ▶ Activating temporary alternative treatment (selection clinic, safe clinic, non-face-to-face treatment, and others) and separating screening clinics from the main building ▶ Expanding ward facilities for confirmed/suspected COVID-19 patients ▶ Operating separately of safety clinics for blood disease patients. Regarding the ward facilities, the entire floor with independent air conditioning was emptied to treat COVID-19 patients, and the ward was divided based on the triage so that the providers could take care of severe cases while separately treating other patients with pneumonia or epidemiological factors.
As a result, the fact that blood hospital treatment was performed normally even during the pandemic gained attention in this journal and its publication was finally approved. During this period, there was no occurrence of COVID-19 in Seoul St. Mary’s Hospital and the number of temporary alternative treatment patients of blood hospital was 749 as of March 2020. While the number of new patients decreased slightly in March 2020, the number of outpatients and inpatients was similar to the one before the pandemic, and it was reported that the number of stem cell transplants was the same.

(From left) Professor Dongwook Kim, President of the Blood Hospital, Seoul St. Mary's Hospital, Catholic University of Korea, Professor Donggun Lee, Director of Infection Control, Professor Sungyeon Cho, the Dept. of Infectious Diseases, Professor Seongsu Park, the Dept. of Hematology.
With Professor Seongyeon Cho (co-first author) of the Dept. of Infectious Diseases, Professor Seongsu Park (co-first author), the Dept. of Hematology, Professor Donggun Lee (the Dept. of Infectious Diseases, corresponding author), Director of Infection Control, Professor Dongwook Kim, President of the Blood Hospital (the Dept. of Hematology, corresponding author), the research team mentioned, “As the COVID-19 pandemic continues globally, each medical institution began to try to prevent the inflow of COVID-19 into the hospital. Meanwhile, Seoul St. Mary’s Hospital established an active response strategy by operating separately a safety clinic in the blood hospital, rather than restricting treatments. That could be the main strategy that the treatments for the blood disease patients could be performed consistently even during the pandemic.”
Professor Dongwook Kim, President of the Blood Hospital, added, “I hope that this thesis will serve as a reference for doctors and patients around the world, whose normal treatment was restricted due to COVID-19, so that the treatment of patients with severe blood disease can proceed without any difficulty.”
The results of this study were published on May 18th in the online edition of the British Journal of Haematology (IF 5.206), a renowned international academic journal.
[Figure 1] The traffic between the patients suspected of COVID-19 and general patients was separated at triage with a questionnaire applied.
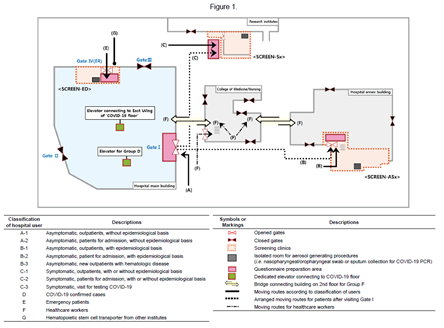
Through triage with a questionnaire, the traveling line of suspected COVID-19 patients was separated from the one of general patients.
[Figure 2] The figure of the comparison in the same month last year with the number of outpatients, inpatients and stem cell transplantation at the blood hospital during the COVID-19 outbreak: the number of new patients in March 2020 is seen slightly decreased but other numbers are similar, which shows that the blood hospital was functioning during the pandemic as normal.
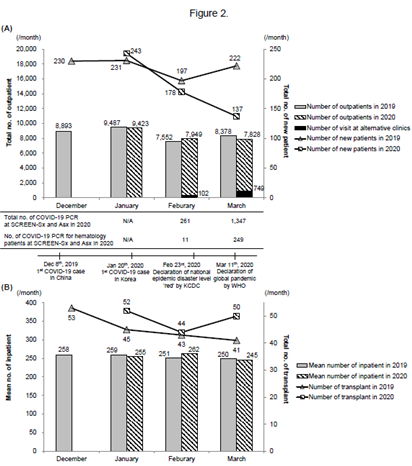
As a result of comparing the number of outpatients, inpatients, and stem cell transplantation at a blood hospital in the same month last year with the period of COVID-19 outbreak, the number of new patients in March 2020 is seen slightly decreased but other numbers are similar. That means that the blood hospital was functioning during the pandemic as normal.
Inquiry